Master Data Management In Healthcare: Benefits & Challenges
Learn about the advantages and challenges of implementing a master data management strategy in healthcare, including improved data quality, more efficient coordination of care, enhanced privacy and security, and cost savings.

Master data management (MDM) is a process and technology that helps organizations manage their core data more effectively. It can help to create a single, accurate view of data across different systems.
In healthcare, where patient data is so often spread across silos both within and between providers, master data management is a critical component of effective administration – though it is not without its challenges.
In this article, we’ll discuss a few of the most significant benefits master data management has to offer the healthcare industry, as well as the unique considerations that still need to be addressed before its full potential can be reached.
How Using MDM Can Result in Improved Data Quality
A major argument for using master data management in healthcare is based on the critical need for highly reliable and accessible data. Like many organizations, care providers often store data across different departments and systems.
This can cause inconsistencies in how data is logged and updated, allow mistakes to fly under the radar, and make it difficult to view data related to a particular subject (for example, details pertaining to a certain process, patient, or piece of equipment) easily and holistically.
This not only puts patients at risk; it can also lead to operational inefficiency, as staff spends an inordinate amount of time and energy trying to collect the data they need.
Master data management, in creating a central repository for key data, provides a framework for data governance: a set of policies and processes to ensure data is of a high quality and accessible to those who need it. This is among the many benefits of using an MDM system.
Under a governance framework, organizations can introduce routine data cleansing and enrichment processes to ensure data is up-to-date, complete, and standardized.
Depending on the size and complexity of the data sets in question, this may be done manually or via specialized software.
However, the lack of a standardized approach is a major challenge in using master data management to improve the quality of healthcare data. There is no single, agreed-upon definition of what data should be included in a master data set.
Healthcare organizations will need to work together to create standards for data inclusion in order to make master data management an effective tool for improving healthcare data quality.
Another challenge is the sheer volume of data. In this industry, data sets are growing at an exponential rate. Any strategy – whether it be selecting a framework for MDM or automating an MDM structure – for master data management in healthcare needs to be based on highly scalable technology and managed by dedicated teams, in order to keep up.
MDM’s Role in Matching Patient Records

A major challenge in healthcare is comprehensively matching patients to their records. This is due, again, to the number of different systems used by healthcare organizations, as well as the diversity of ways in which patient data can be entered into those systems.
Mismatched patient records can lead to a number of serious issues, including misdiagnosis, delayed treatment, conflicting treatment plans, and inefficient use of healthcare resources.
Free Book: Practical Guide to Implementing Entity Resolution
Interested in implementing an in-house record matching solution with your own development team without using any outside vendors or tools?

Creating a framework for master data management in healthcare would enable the effective linking of patient records, creating a single, integrated view of patient data that could be used by all healthcare organizations. This would allow for better coordination of care and would make it easier to track patients across the healthcare system.
For example, if a patient is seen by a primary care physician and then goes to the emergency room, their records would be linked and the ER would have access to the patient’s medical history.
Currently, the most significant challenge in linking patient records is the lack of a common identifier – that is, a single, unique attribute that can be used to reliably link all relevant data to a single patient.
The Health Insurance Portability and Accountability Act (HIPAA) requires that all patient information be kept confidential, which means that healthcare organizations cannot share patient information without the patient’s permission.
This makes it difficult to create a central database of patient information. One way to overcome this challenge is to use a unique patient identifier (UPI, a unique number that is assigned to a patient when they are first seen by a healthcare provider. This number would then be used by all subsequent healthcare providers to identify the patient.
Another way to manage patient data is through the use of a Master Patient Index (MPI). An MPI is a central database that links together all of the records for a patient that are held by different healthcare organizations, creating a complete picture of that patient’s health.
Implementing either unique patient identifiers or a Master Patient Index would require a high degree of coordination among healthcare organizations across the country, but may go a long way toward improving care. At this rate, providers may look for different record linkage tools or choose to build one for themselves.
The Data Privacy and Security that MDM provides
Given the sensitive nature of healthcare data, it is essential that proper security measures are in place to protect it.
By providing a single, centralized view of an organization’s data, master data management can enable the identification, tracking, and management of sensitive data. This helps reduce the risk of data breaches and makes it easier to ensure compliance with data privacy regulations.
MDM’s effective data governance framework in place enables healthcare providers in ensuring that only authorized individuals have access to sensitive information. Accidental or unauthorized access to data, as well as unauthorized sharing, will be easy to spot.
When a breach does occur, master data management can help minimize the impact by providing a single source of truth for data. This can help reduce the spread of inaccurate information and make it easier to identify which data was compromised.
Helping Providers Save Money
Having a master data management can also help healthcare providers save money in a variety of ways.
By creating an accurate view of patient information, it’s easier to identify areas where costs can be reduced. For example, it can be easier to track care gaps and ensure that patients are receiving the right treatments at the right time. This helps limit unnecessary tests or treatments while ensuring that all necessary care is provided in a timely manner.
Additionally, MDM makes it easier to streamline administrative processes such as billing and insurance claims processing which can result in cost savings over time.
Healthcare MDM Wrapped Up
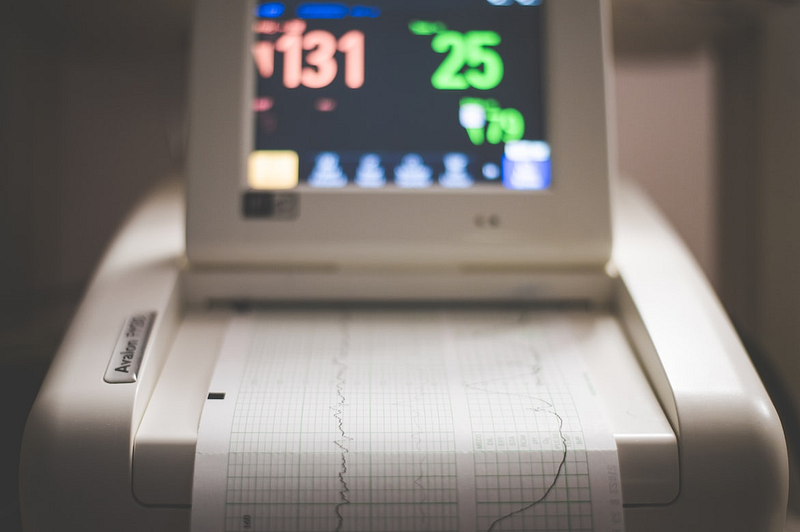
Despite its challenges, implementing a well-designed strategy for master data management in healthcare may have a significant impact on the privacy, security, and quality of healthcare data. By providing a centralized view of critical information, master data management can help the industry improve data quality, accessibility, and security.
The healthcare industry may also benefit from understanding how master data management works hand-in-hand with enterprise resource planning. This is done to ensure that aside from having “one source of truth” for an organization, they can also optimize the gathering and cascading of data.
If you are looking to improve the quality of your data but don’t have the time or resources to create a master data management program, look no further than RecordLinker.
Our data integration and management platform can quickly connect disparate data sources, identify and deduplicate records, and keep your data clean and up-to-date. Moreover, we have other related articles that you might be interested in.


